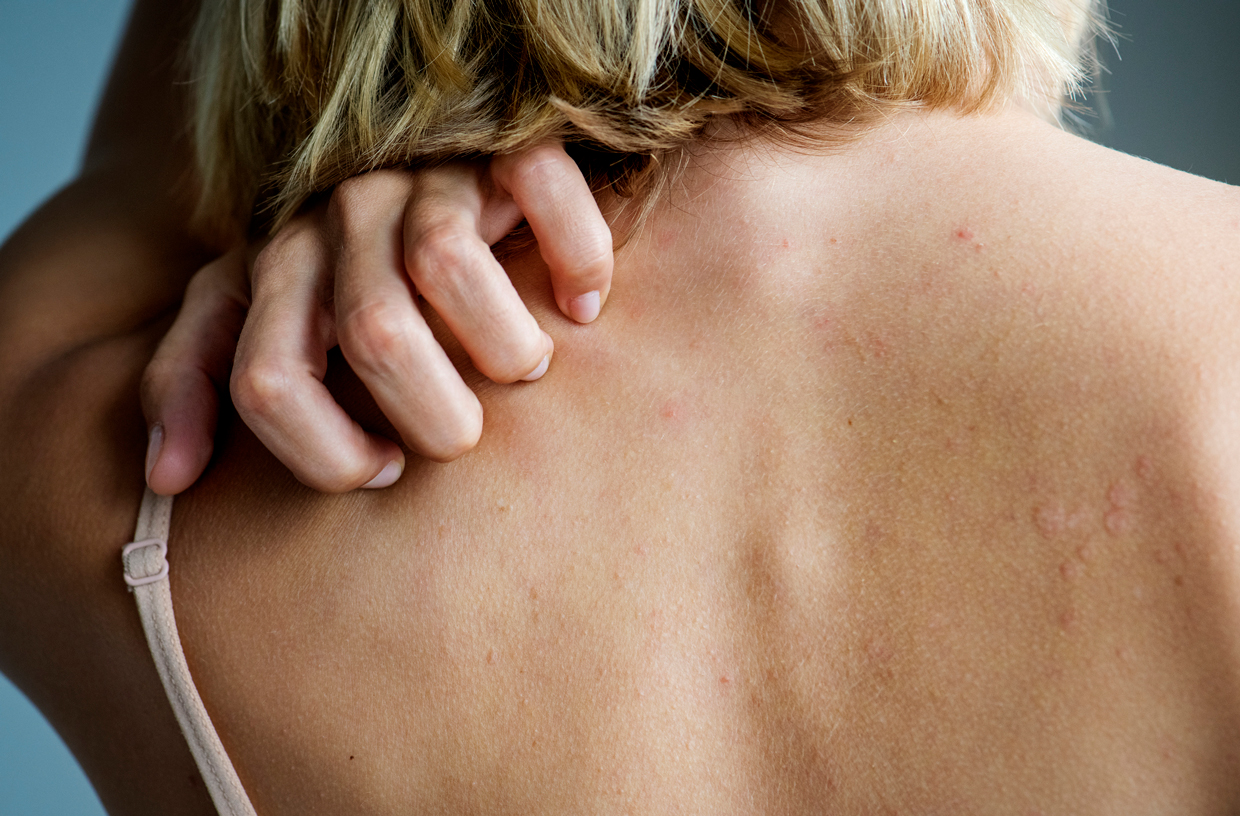
Dermatitis is a common skin condition that presents itself in many not-so-fun ways — from when you’re a baby (like diaper rash) to adulthood (e.g. dandruff). It’s a general word used to capture a lot of reactions that your skin might be experiencing. “It’s basically an umbrella term that refers to inflammation of the skin and essentially it’s associated with what people would consider a typical rash of the skin,” says Dr. Marisa Garshick, a board-certified dermatologist and Clinical Assistant Professor at Cornell University. If you’re curious whether or not a reaction on your skin is dermatitis, our pro gives us the scoop on what to look for — before you get it checked out by your own dermatologist, of course.
What are the types of dermatitis?
Dermatitis isn’t contagious or dangerous, but moderate or severe cases can make your skin feel uncomfortable. There are several types of dermatitis but the most common are:
- Atopic dermatitis: “This is what most people consider to be eczema,” says Garshick. It can affect you at any age and it doesn’t necessarily mean you’ve had exposure to something you’re allergic to.
- Contact dermatitis: “Sometimes we divide this subtype into an allergic contact dermatitis versus an irritant contact dermatitis. An irritant contact dermatitis happens when someone is exposed to something in sufficient quantities and it can irritate the skin. For example, we can develop irritation when we wash our hands. When people actually experience dryness of the hands, oftentimes that’s actually an irritant of contact dermatitis just because of all the hand washing or sanitizer that people are using. Allergic contact dermatitis is describing an event where somebody gets exposed to a certain ingredient or component of a product and subsequently develops a rash as a result. It can take several days for this type of dermatitis to appear after exposure,” she says.
- Seborrheic dermatitis: “For many people, this is related to dandruff. It’s usually an inflammation of the skin on the scalp. This inflammation relates to where those hair-bearing oil glands are — like the scalp, the eyebrows, and sometimes on the chest area. It can appear similar to these other types of dermatitis in the sense that you see these red flaky patches, but the mechanism is different. So, it’s not necessarily dry skin that you’re seeing, it’s actually just acknowledging this inflammation as a result of oily skin. Though it looks dry and flakey, it won’t go away with more moisturizer — we address it by targeting the inflammation, the yeast, and trying to remove some of that excess oil,” she says.
“Though dermatitis isn’t life-threatening, because this inflammation of the skin can disrupt the skin barrier, it can make it more susceptible to fungal or yeast infections, bacterial infections like staph aureus, or a viral infection like herpes,” she says.
What causes dermatitis?
Dermatitis isn’t contagious or dangerous, but moderate or severe cases can make your skin feel uncomfortable.
“We don’t always know the causes, but there’s definitely a hereditary component to it. We call certain people having what’s known as an atopic diathesis — or a predisposition — to these types of inflammatory conditions. For many people, atopic dermatitis develops in childhood, even as babies. In some cases, people grow out of it, and in other cases, it sticks with them. Some people can develop it later in life. Lifestyle-wise, it can worsen in the winter months when the skin gets more dry or gets aggravated by stress. Studies show that the increase of stress during the pandemic has played a role in dermatitis, rosacea, and acne. Some people may find that there are triggers for them individually. For instance, certain fabrics can be aggravating on the skin like wool during the dry winter months. If somebody’s sensitive to jewelry or allergic to jewelry and they have earrings that contain metal like nickel, they may experience a rash around their ears. Another example is that people may be allergic to a component in nail polish. Even though they may not necessarily see the rash on their hands, you can experience a rash around your face whenever you touch your face with your fingertips — the nail polish could be transferred to your skin. A lot of the time, dermatitis is mostly triggered and worsened by just having drier skin.”
What are the usual symptoms of dermatitis?
“Itchiness, dry skin, rash, redness, and flaking can occur anywhere on your body. As you get into the different subtypes, there are more descriptive ways to talk about the symptoms depending on how long the rash has been there. For example, sometimes we’ll call it acute, which means it came on suddenly. It can appear almost the way poison ivy tends to immediately blister or cause weeping of your skin. There’s also subacute dermatitis, which means your condition has possibly been there for a few weeks and that tends to be more red with flaky patches or plaques of the skin. Then there’s a more chronic form of dermatitis, which refers to the fact that it’s longer duration. It can trigger changes in the skin where the skin actually becomes thicker in appearance and you have an accentuation of what we call the skin markings. You don’t easily see the lines that are normally present in the skin, but when the skin gets thicker and the medical term for it is something called lichenification,” says Garshick.

Does dermatitis present itself differently on deeper skin tones?
“In many cases, we use the term red or pink patches to describe symptoms, but in those who have darker skin, it can appear as more of a purplish color or even hyperpigmented, which basically refers to a brown discoloration that can initially appear. You can still experience flaking, you could still experience blistering, but it’s usually just the color that may appear different where inflammation in somebody with lighter skin is more likely to appear red and pink, where in somebody with darker skin, it may just appear as a darker version of their normal skin tone,” says Garshick.
Does dermatitis get confused for other skin conditions?
“A lot of times, patients will come in and say ‘I have hives’ because most patients think of anything that they see on their skin as hives. In general, however, hives tend to be more smooth at the surface and more transient. Hives tend to come and go whereas dermatitis is usually pretty persistent. Once dermatitis is there, it’s not going to go away unless we intervene with treatment or we give it a week or a few days to go away on its own. But, dermatitis won’t disappear within the same day the way hives can. Dermatitis also has some overlap in symptoms with psoriasis and can be confused with dermatitis. Fungal infections can also appear red and scaly. So, even though the origin is not sort of true dermatitis, there can be some overlap there as well,” she says.

How does a dermatologist confirm it’s dermatitis?
“Your dermatologist will be trained to recognize and identify the specific patterns of dermatitis. For example, with psoriasis, the flaking that somebody might experience might be different from the flaking you see in dermatitis — though, to a typical patient, they make look the same. Dermatitis can also be determined by the location on your body. For example, eczema or atopic dermatitis may follow certain patterns where it most commonly affects the flexural areas, which are behind the knees and on the inner aspect of the forearm. Whereas, psoriasis is usually the extensor meaning front of the knees and the elbows. There are also more definitive tests like a skin biopsy that can give more information on what might be triggering your rash or patch testing to see if it’s contact dermatitis,” she says.
How can you treat dermatitis?
Medication/prescription
“Usually there will be some form of topical anti-inflammatory cream, ointment, or lotion that can treat your dermatitis. For pretty much any subtype, using a steroid can be an effective option to treat topically. In some cases, for example, for atopic dermatitis, there may also be medications that you can take by mouth or as an injection that can also be helpful. For contact dermatitis, similarly, it’s not the same pill or injection, but you can also do a pill to calm down the immediate inflammation. There are differences because even though dermatitis is encapsulating all of them, there are nuances that make each treatment a little different for each condition. For instance, with eczema, you really want to address dry skin and use moisturizing products and gentle cleansers. While with seborrheic dermatitis, it’s really more just a matter of washing the hair frequently to get rid of the excess oil using antifungal or anti-dandruff shampoos,” she says.
Over-the-counter
“Since the skin barrier is considered impaired or disrupted, anything that’s going to help restore, protect, or strengthen that skin barrier can be effective. I recommend products containing ceramides or niacinamide to help repair the barrier and soothe the skin,” she says. [Editor note: Sunday Riley ICE Ceramide Moisturizing Cream uses the power of ceramides to replenish the skin barrier with hydration.] “Protective ingredients are occlusives, so products like Vaseline, which has a petroleum base to it. In terms of seborrheic dermatitis, that’s the only one where you probably wouldn’t want to necessarily do that. Since your skin is already sensitive from dermatitis, you want to avoid any harsh, active ingredients. This definitely includes exfoliants for the time being. Even though the skin is flaky, it doesn’t necessarily mean you need something to help the skin flake off. You actually want to target the inflammation instead and allow that to go down before you worry about flakey skin — otherwise, it makes your dermatitis worse. Avoid abrasive physical scrubs, harsh soaps, and exfoliating acids. Whenever you’re experiencing a flare of dermatitis, you do want to be as gentle as possible on your skin,” she says.
We only recommend products we have independently researched, tested, and loved. If you purchase a product found through our links, Sunday Edit may earn an affiliate commission.