Our hope for summer skin is glowy and sun-kissed, but the truth is that the high temperatures and ample sunlight can cause a host of skin woes. I know this firsthand, unfortunately, because I got poison oak (on my face) on a recent camping trip after hugging (read: smooshing my face into) my dog, who had apparently run through a patch of the poisonous plant.
To uncover some of the most prevalent summer skin issues, I talked with Michele Farber, M.D. a dermatologist from Schweiger Dermatology Group. She shares some of the most common skin issues she sees in her patients during the summer months, and because we would never leave you hanging, we have tips on how to treat and prevent these skin conditions, too.
Summer Skin Issue: Acne

I thought one day my acne would just pack its bags and leave for good, but it does still show up on my adult face, particularly in the summer months. Sweating and excess oil production may exacerbate acne because sweat and oil cling to dirt, pollution, even sunscreen, causing your pores to clog (which is when acne forms). If you notice you are breaking out more in the summer months, or if you are lucky enough to live somewhere that is warm all year, Farber recommends using “a gentle face wash twice every day and always after workouts or sweating. Make sure your products are non-comedogenic or oil-free.” There is no reason to cleanse more than twice a day. In fact, over-cleansing may make acne worse because skin dries out and produces more oil to compensate.
I know it is tempting (and I am definitely guilty of it at times) but do not pick or pop your pimples. Try not to touch them at all, as this will delay healing and potentially push bacteria further into the skin.
And while it may seem counterintuitive to lather sunscreen on top of acne, Farber says, “sunscreen is a must! UV exposure can cause hyperpigmentation to last after acne heals. SPF and sun-avoidance like hats are also important.” You can opt for a mineral sunscreen that may be more gentle on the skin and definitely better for the environment.
Summer Skin Issue: Prickly Heat
Prickly heat is a rash on the skin that stings or “prickles” and is sometimes called miliaria or heat rash. It is typically caused by clogged sweat ducts in hot weather, which means sweat can’t leave the skin and evaporate (this is what it is designed to do as a way of cooling the body) and instead stays trapped in the body causing itching and irritation. Farber suggests that you make sure that your clothes are light and breathable, and if possible, stay inside during the hours of peak heat. If you do get prickly heat, make sure to change out of sweaty or wet clothes, which can aggravate the rash. Farber says oatmeal baths can also help.
Using portable fans (anyone remembers the great Squeeze Breeze phase of 1995 or was that solely restricted to my local day camp?) and staying in a cool environment “can hasten the resolution [of folliculitis] and prevent breakouts.”
Summer Skin Issue: Sun-Induced Rashes
Phytophotodermatitis is a rash that occurs from sun exposure after a person has to contact with certain plants (or essential oils) including lime, figs and fragrances. It is caused by exposure to furocoumarins, which are chemicals found on plant surfaces that when activated by UV rays can cause a reaction. Bergamot and citrus essential oils may also induce a photosensitive reaction, which explains why I burned in the sun after taking a bath with grapefruit oil in it. Of phytophotodermatitis Farber says, “It clinically can look like a sunburn and when deeper there are blisters. Anyone who is exposed to a predisposing chemical in sunlight typically will experience this rash. It can be prevented by avoiding common causes, like limes, while exposed to the sun.”
Farber adds that “certain people develop a hive-like reaction in the sun called polymorphous light eruption. Certain medications can also make you more sun-sensitive, ranging from antibiotics to pain medication, so check your medications as well and review them with your dermatologist.”
Though the rash may look and feel serious, these breakouts can be easily managed with a dermatologist-prescribed regimen.
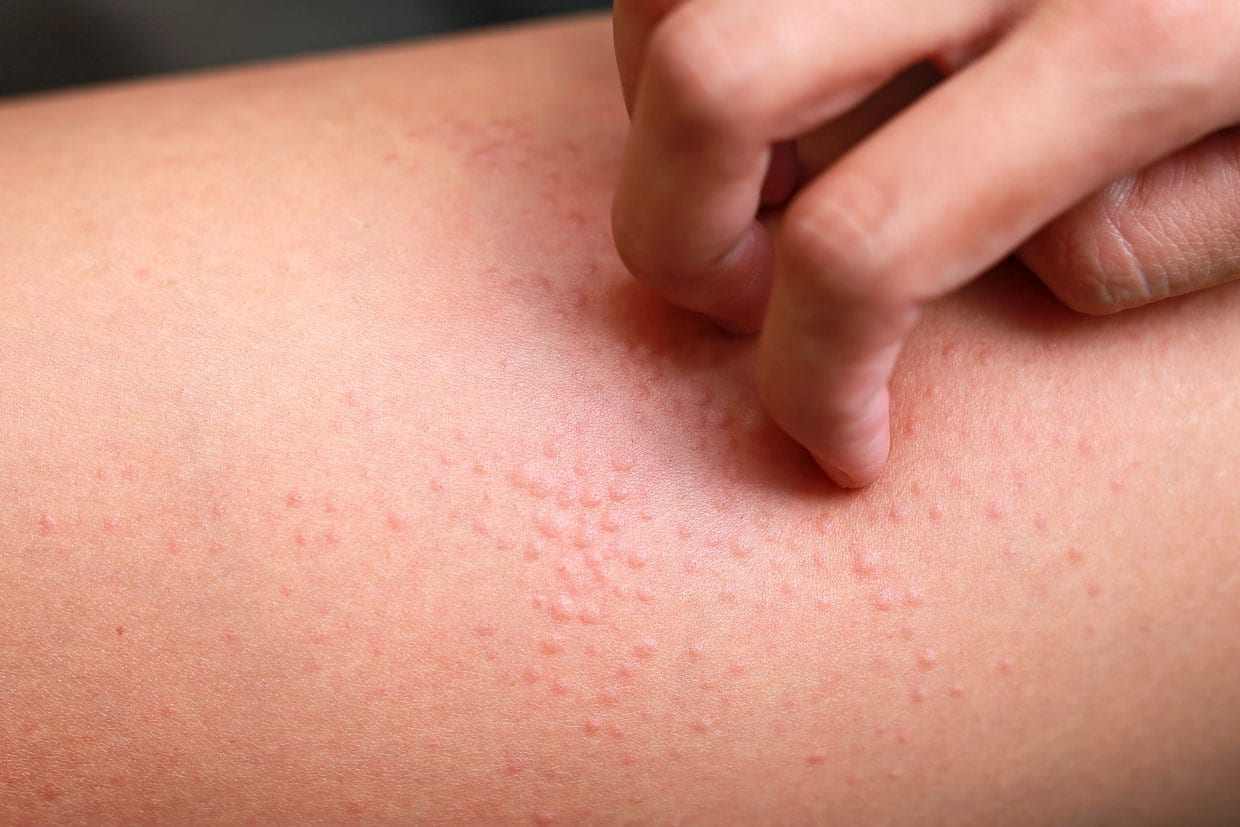
Summer Skin Issue: Eczema Flare Ups
Some people who have eczema will see their symptoms worsen in the summer months because the heat and higher humidity levels can exacerbate symptoms, according to the National Eczema Association. There are also common allergies that can aggravate skin and eczema may also be worsened by stress or sweat. If you are prone to eczema or sensitive skin, below Farber shares her suggestions for dealing with summer flare-ups:
- Shower immediately after swimming and do not sit outside in a wet bathing suit. Sitting in a damp bathing suit can trap bacteria and promote the growth of yeast, both of which can worsen eczema. Chlorine can also worsen eczema, so it is best to shower it off as soon as possible.
- Choose a medium setting for the air conditioner. Very low settings can contribute [to] dryness because air conditioning dries out the air and the skin. Adding humidifiers can help.
- Moisturize consistently! Pick a fragrance-free moisturizer, as well as thicker products like cream over a lotion for better hydration.
- Pick a mild, fragrance-free cleanser, keep showers short and turn the temperature down to lukewarm. Artificial fragrances can aggravate eczema and long, hot showers may increase skin’s dryness and irritation.
Summer Skin Issue: Melasma
Melasma is a skin condition that causes areas of the face to darken into a shade of brown or gray. It most commonly occurs on parts of the face that the sun hits: forehead, bridge of the nose, upper lip and chin (think places you apply bronzer). Though melasma is thought to be caused in part by hormones — according to the American Academy of Dermatology, melasma is sometimes referred to as “the mask of pregnancy” — the condition gets more pronounced in the summer or if you live in a place where the sun shines regularly.
UVA rays penetrate deeply into the skin and can cause premature aging. UVB rays damage the superficial outer layer of the skin and can cause burning or skin cancer. So, Farber recommends that people with melasma “choose a broad-spectrum sunscreen that covers UVA and UVB. This pigment is best prevented by a physical sun blocker like titanium dioxide or zinc oxide with a minimum of SPF 30 plus tint.”
She adds that “hormonal changes can also contribute to this type of pigment change. Discuss medications and other factors that may be flaring melasma with your provider as well as treatments to lighten it.” Treatments for melasma include chemical peels, microdermabrasion, dermabrasion, laser treatments or light therapy.

Summer Skin Issue: Folliculitis
Folliculitis is a common skin condition that looks like acne but is not. It can be caused by razor burn, hot tubs, yeast or if the follicles become infected by bacteria, most commonly staph. The red bumps can be itchy or sore, and if you get folliculitis on a recurring basis, you may need to see a doctor. Farber says folliculitis can worsen in the summer because of “sweating, humidity and rubbing.”
Here is how Farber suggests preventing it:
- Always change out of tight clothing, especially after the gym or wet bathing suits after swimming.
- Be careful with hair removal — always use shaving cream, sharp razors and never pick. If ingrowns are a consistent problem, consult your provider about laser hair removal.
- There are rarer types of infections that can present like folliculitis. These include pityrosporum folliculitis, in which yeast overgrows in hair follicles, and hot tub folliculitis from improperly maintained hot tubs. While these typically require prescription medications, they can be easily treated.
- Systemic causes as well as medications can contribute to folliculitis, so consult your dermatologist if your bumps are not resolving.
We only recommend products we have independently researched, tested and loved. If you purchase a product found through our links, Sunday Edit may earn an affiliate commission.















